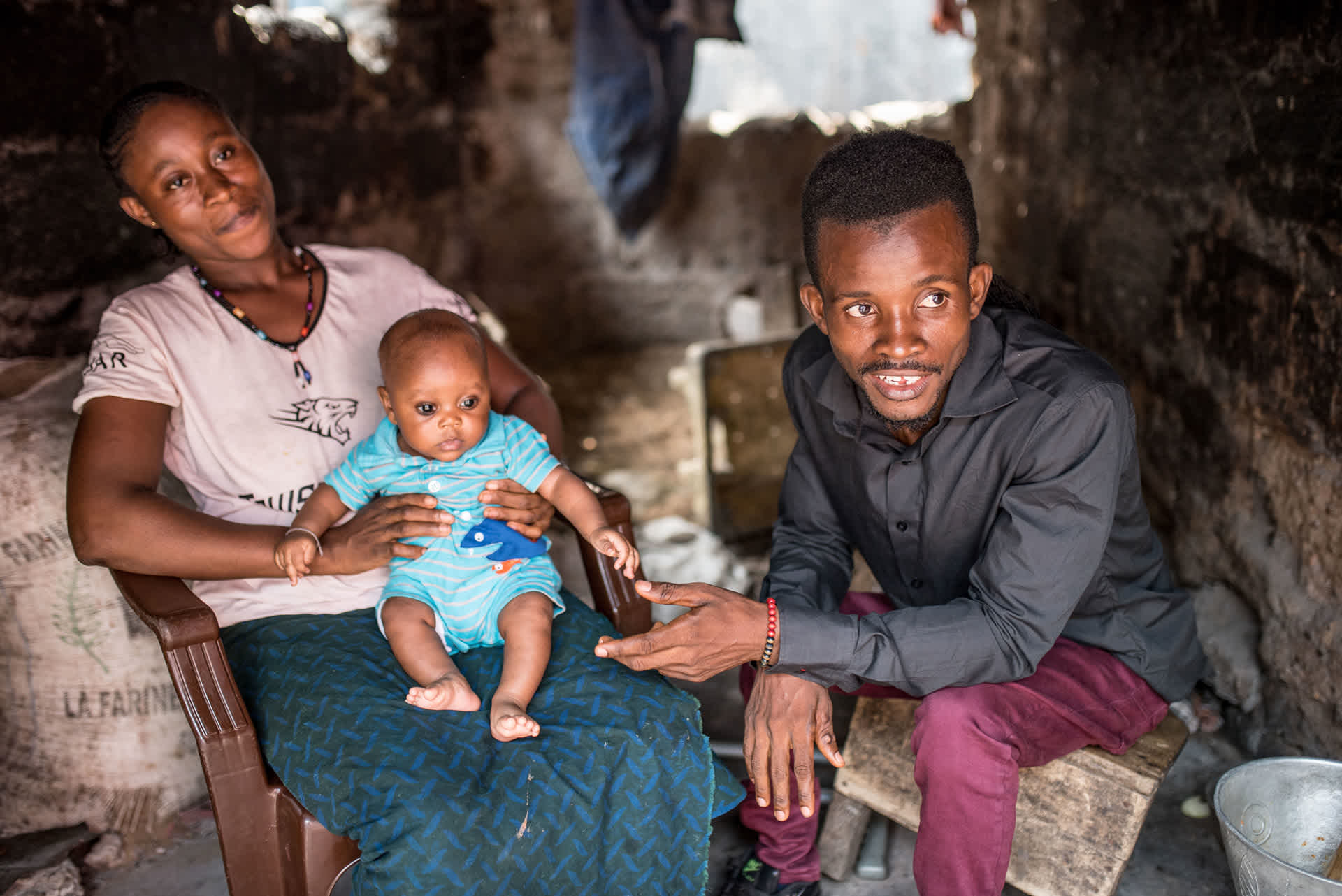Our impact and learnings
Over 6.3 million people were reached across five years as a result of the Comic Relief and GSK partnership.
In 2015 there were 214 million cases of malaria worldwide, with 438,000 deaths from this preventable disease.

In 2016 we joined forces with GSK to form the Fighting Malaria, Improving Health partnership, focusing on disease control through strengthening health systems.
At the beginning of the partnership, we spoke to governments across Africa and the Greater Mekong area - specifically some of the countries that were most affected by malaria - and we learned that more interventions were needed to prevent, diagnose, and treat malaria.
We set out to complement and enhance existing national strategies to tackle malaria, providing funding where it was needed most. Focusing on four core pillars of work.
Read about our four pillars of work

There are 6 main areas of impact from the partnership
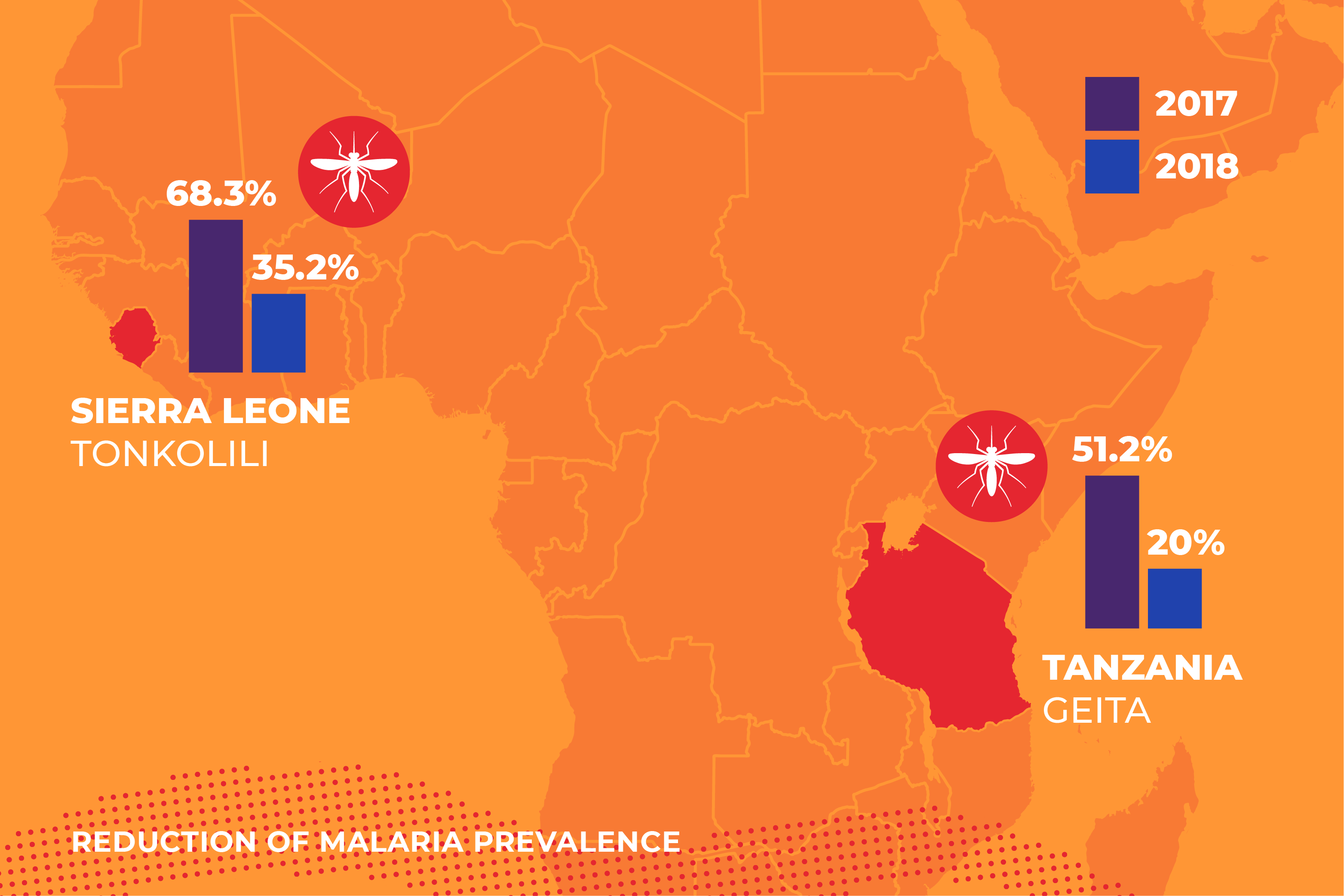
1. Reduction in malaria prevalence in intervention areas.
In 2017 in Sierra Leone, malaria prevalence in Tonkolili was 68.3%. The 2020 malaria indicator survey conducted by the National Malaria Control Programme (NMCP), estimated malaria prevalence in Tonkolili at 35.2%. The Empowering Communities to Treat and Prevent malaria (TAP) project was implemented by Concern Worldwide in 25 out of 91 communities in Tonkolili and had a significant influence on community behaviour.
Similarly, the prevalence of malaria in Geita region of Tanzania was over 50% in 2017 at the beginning of the Association of Private Health Facilities in Tanzania (APHFTA) malaria project and at the end in 2021 measured below 20%.
2. Increased malaria awareness and knowledge leading to improved health seeking behaviour.
Community level approaches which amplified local voices and experiences saw some quick wins.
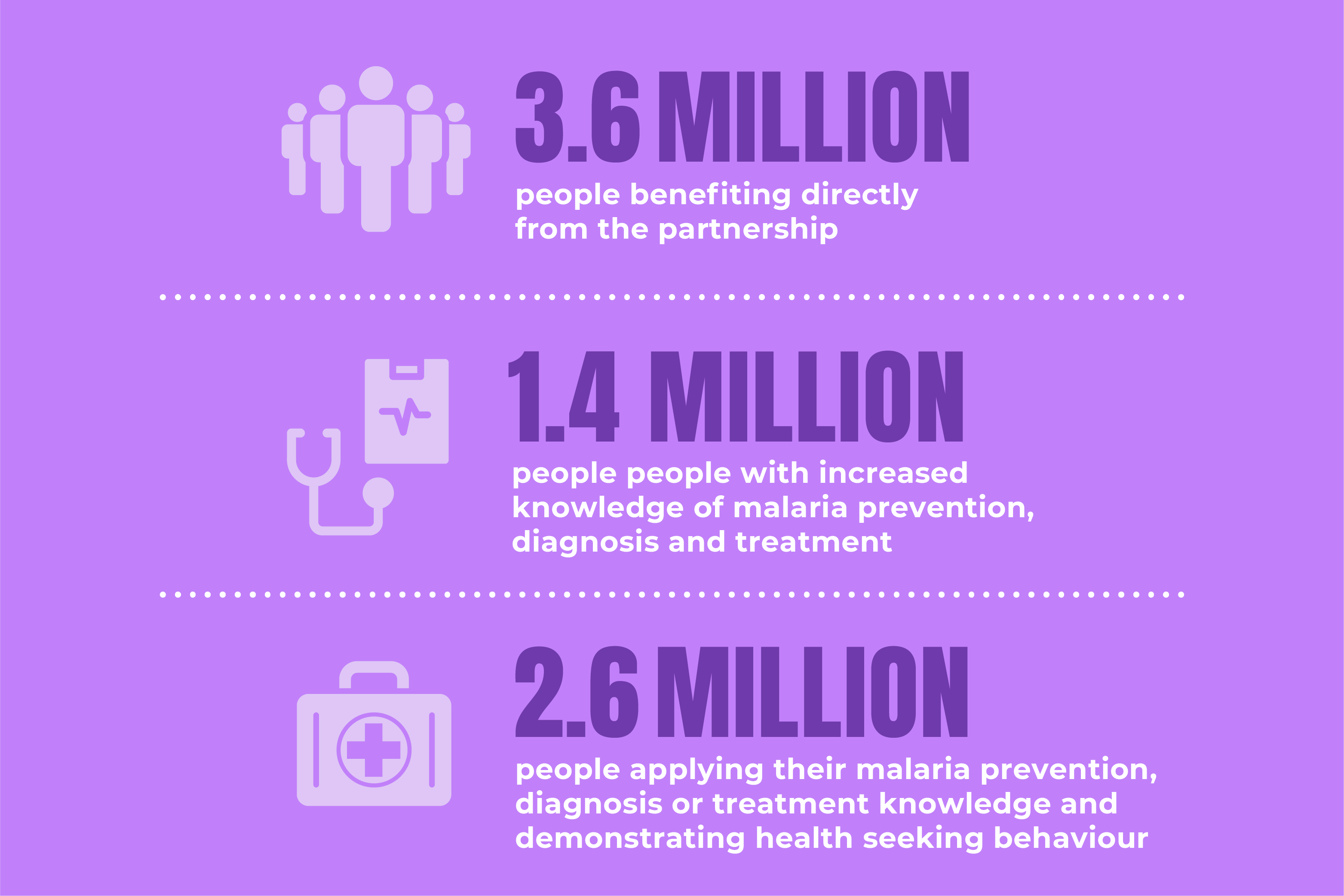
3.6 million people benefiting directly from the partnership
1.4 million people with increased knowledge of malaria prevention, diagnosis and /or treatment
2.6 million people applying their malaria prevention, diagnosis or treatment knowledge/demonstrating health seeking behaviour.
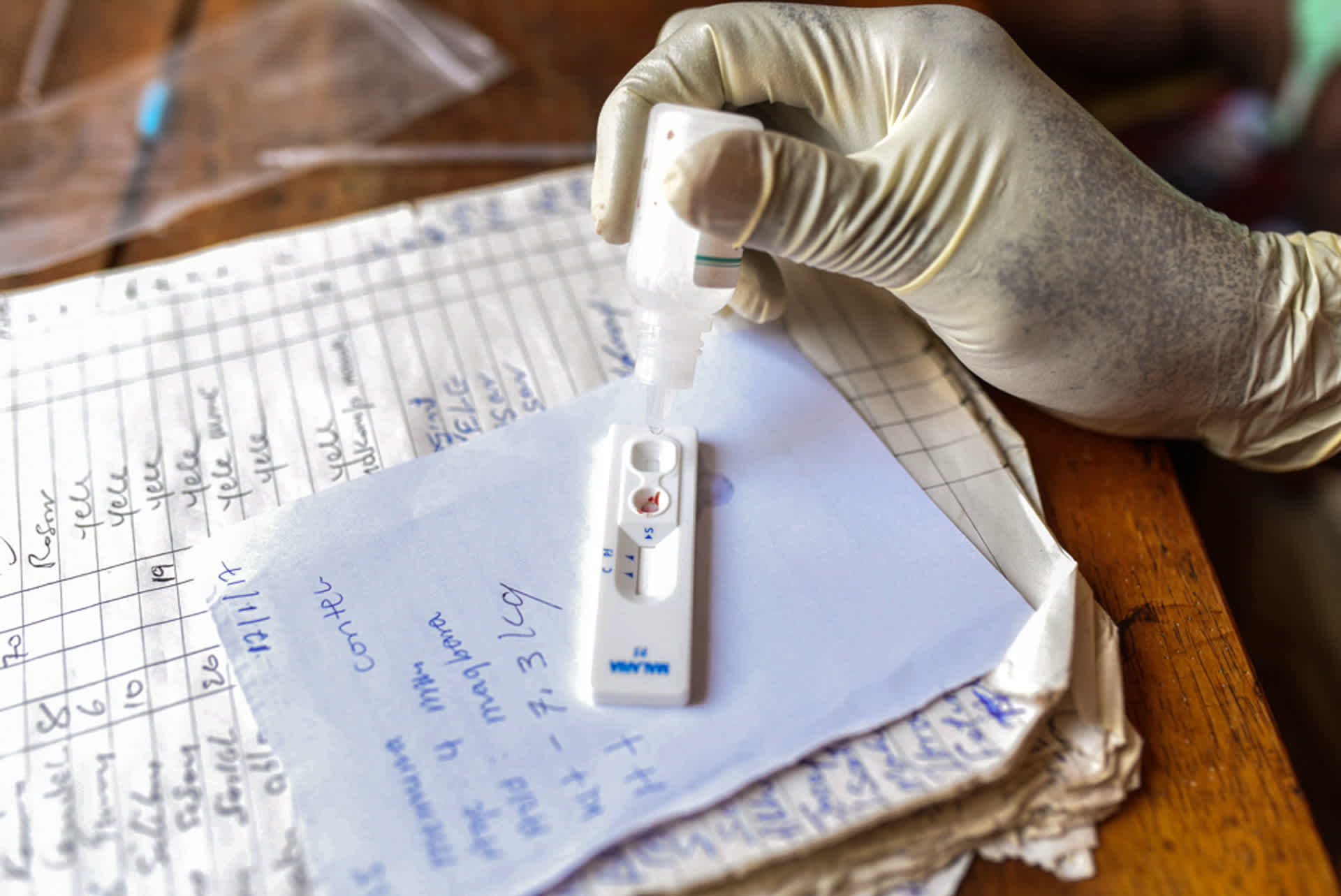
3. Improved capacity of health workers in geographies of intervention.
This was a key change by national and provincial government stakeholders and our funded partners and was attributed to extensive trainings and frequent supervisions supported by our funded partners.
1.6 million people accessed improved diagnostic services in Tanzania, Sierra Leone, GMS and Ghana due to the partnership’s interventions.
9.6K people accessed improved quality of treatment services across the partnership’s five focal geographies.

4. Private informal sector was strengthened and integrated better into the formal health system.
A core innovation of the partnership was the work we did with the private informal sector - partnerships with the formal private sector are more usual and integration of data from private sector into the public sector is atypical. During the scoping phase we identified trends in the way people approached health care. By working with the informal sector we were accessing the first point of call when falling ill and this was a pivotal part of the partnership’s success in strengthening the diagnosis and treatment of malaria.
The private informal health sector in several countries were strengthened by the funded projects – private community providers in Cambodia; private outlet providers in Myanmar; accredited drug dispensing outlets (ADDOs) and autonomous laboratories in Tanzania; and licensed chemical sellers in Ghana.
Capacities were increased, referrals between private and public parties were improved; and information management and surveillance systems were strengthened. The integration of private sector data into public sector data was an important gap filled by the partnership.
5. Strengthened health systems.
In Sierra Leone, the National Malaria Control Programme (NMCP) scaled up International Rescue Committee (IRC)’s project from 38 to 100 pharmacies and used the model for other healthcare initiatives beyond Rapid Diagnostic Tests (RDTs) and the malaria sector.
In Tanzania, the Clinton Health Access Initiative (CHAI) project influenced the NMCP to position the intervention for scale up via a Global Fund Application. The integrated approach - which led to the expansion of a new modified drug register, introduced by CHAI, beyond the four project intervention regions to seven more regions in collaboration with the NMCP and other partners - was a plus for health systems strengthening.
Capacity was also strengthened beyond the malaria sector. In Myanmar, Population Services International (PSI) worked in 16 project townships located along the Indian border where the government was not able to support. The project strengthened the capacity of more than 850 community private providers in malaria and TB, HIV, Leprosy, Diarrhoea, and infectious diseases.
6. Communities at the heart of what we do.
Our advocacy and communications strategy supported the communities in telling their own stories and sharing their own experiences. We connected with a range of communities through the projects and created over 70 case studies and a series of films all supporting the goal of spreading awareness.
Our advocacy grants contributed to setting the malaria agenda at national and international levels. The grants mobilized important political, social and (to an extent) financial verbal commitments from decision makers and political leaders. We remain hopeful that these commitments are soon translated to significant national level policy change or release of funding to the sector.
Our funded partners were effective in securing policy change. PSI contributed to changes made to the Myanmar national malaria advocacy policy - a new advocacy policy for the national programme was introduced in order to raise funds through the regional advocacy workshop for Cambodia, Lao and Myanmar. The Community Based Management of Acute Malnutrition (CMAM) Surge approach used by Concern Worldwide in Sierra Leone was adopted in the country’s next 5-year malaria strategy.
COVID-19 limitations and adaptations
In 2020 our partnership was met with the challenge of the COVID-19 pandemic. This was especially the case for our advocacy funded partners. Convenings, meetings were disrupted by the pandemic and the subsequent national emergency declarations in the different geographies.
On a national, provincial and local government level all stakeholders’ attention turned to managing the pandemic. Ministry of Health staff became focused on addressing the health challenges resulting from the pandemic and malaria ranked low on the priority scale. The funded projects adapted in different ways. Advocacy groups used online communications to reach out to prospective targets. Funded partners collaborated with government stakeholders to respond immediately to the outbreak. Funded partners secured approvals from Comic Relief to re-assign their budgets to purchase emergency Personal Protective Equipment (PPE). The funded partner Health Poverty Action (HPA) was the first NGO to get PPE for malaria workers in their target areas in Cambodia. Kings College London (KCL) in Sierra Leone supported the re-establishment of the infectious disease unit built during Ebola time and quickly managed the COVID-19 testing with the laboratory staff in Connaught. In Ghana, Anglican Diocesan Development and Relief Organization (ADDRO) intensified their household visit strategy, supporting volunteers and project officers to implement this safely. ADDRO also received support from Comic Relief to help procure PPEs for facilities in their intervention communities, the Ghana Health Service, volunteers, and ADDRO staff.